Taking medications long term requires strong discipline and motivation; however, people often cite time management as their number one barrier to medication adherence. Most commonly, this means forgetfulness, but it can also be from the lack of a medication-taking routine, a complex medication regimen, no pill box or planner, or a busy schedule. A recent study by Intermountain Healthcare in Salt Lake City, Utah, set out to determine if the “nudge theory” could help overcome time management barriers.
The nudge theory was established by 2017 Nobel Prize recipient Richard Thaler and was originally applied to the field of behavioral economics. Thaler’s nudge theory showed that humans do not always act rationally and sometimes need a “nudge” to make better decisions.
Intermountain Healthcare’s 12-month study, titled “Improvement in Medication Compliance Through the Implementation of Personalized Nudges: the ENCOURAGE Trial,” included 186 participants on statin medications.[1] The study participants were randomized into two groups; one group received standard care, while the other group received “nudges,” or personalized engagement based on the participant’s profile.
The study found that participants who received the personalized nudges were more likely to take their medications and had a higher percentage of the proportion of days covered (PDC), at 80%. PDC is a measurement of medication adherence that is calculated by dividing the number of days a drug is dispensed for by the number of days the patient has the prescription. They also found that participants in the control group—those who didn’t receive any reminders—had gradual declines in PDC over the course of the study.
The Nudge Theory in Action
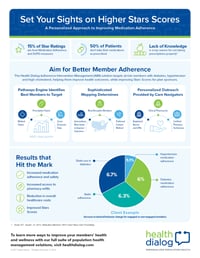
Health Dialog’s medication adherence programs “nudge” members through targeted and personalized engagement. We identify members at-risk for medication non-adherence by engaging the Pathways Engine, our predictive analytics and machine learning platform. Our Pathways Engine utilizes over 600 data points, incorporating medical and prescription claims history and socio-economic factors, as well as other clinical identifiers and care gaps, to ensure we select the most appropriate members to target. Our specially trained Care Navigators then perform “nudges.” Care Navigators identify barriers to adherence and establish a personalized care plan to support intrinsic motivation and help members overcome these barriers.
We recently launched a program focused on increasing medication adherence across a large Medicare Part D population. In the nine-month evaluation period, over 69,000 members were contacted for personalized coaching and 92% of those reached by phone were receptive. Additionally, the study analysis uncovered higher PDC rates for the coached population when compared to the non-coached population:
- 5% higher PDC for diabetes medications
- 9% higher PDC for statins
- 3% higher PDC for hypertension medications
Both the Intermountain Health clinical trial and Health Dialog’s experience demonstrate how a personalized nudge can make a real impact on improving medication adherence.
[1] Intermountain Medical Center. (2019). ‘Nudging” heart patients to take their statins leads to better adherence and better outcomes. ScienceDaily. https://www.sciencedaily.com/releases/2019/11/191114075549.htm.